Never miss a problem with calcified bone detector
Medical imaging often struggles to reveal subtle abnormalities hidden behind dense bone structures. A calcified bone detector uses advanced algorithms to highlight these obscured regions. Radiologists gain sharper diagnostic accuracy. Imaging technicians benefit from faster workflows. Patients receive precise diagnoses and timely care.
What is Bone Suppression Software?
Definition and Purpose
Bone suppression software uses advanced algorithms to digitally remove or reduce the appearance of bones in radiographic images. This technology allows radiologists to view soft tissue structures with greater clarity, especially in areas where bones often obscure critical details. The main goal centers on improving diagnostic accuracy and efficiency in medical imaging.
Note: Bone suppression software does not require additional X-ray exposure or extra equipment. It generates supplementary images automatically, supporting faster and more confident decision-making.
The table below summarizes the core functions and intended outcomes of bone suppression software:
| Function/Outcome | Description |
|---|---|
| Enhanced Diagnostic Confidence | Enables accurate diagnoses more quickly and confidently. |
| Improved Decision-Making Support | Provides extra soft tissue images without extra X-ray dose or time. |
| Efficient Workflow | Produces bone-suppressed images automatically, saving time and resources. |
| Accelerated Exam Performance | Shortens patient wait times and increases daily patient throughput. |
Difference from Traditional Imaging
Traditional imaging methods often struggle with overlapping bone and soft tissue, which can hide important abnormalities. These methods rely on assumptions about bone structure and frequently require manual adjustments, increasing the risk of human error.
The following table highlights key differences between bone suppression software and traditional imaging techniques:
| Feature | Bone Suppression Software | Traditional Imaging (Dual-Energy X-Ray) |
|---|---|---|
| Method | Algorithm-based | Physics-based |
| Performance | Sensitive to patient positioning | Consistent across various views |
| Versatility | Limited to specific views | Applicable to multiple body parts |
| Accuracy | Estimates soft tissue appearance | Physically separates bone and soft tissue |
| Nodule Detection | May miss some nodules | Detects nodules fully obscured by bone |
Traditional imaging also faces limitations such as occlusions from bone structures and the need for manual intervention. Bone suppression software addresses these challenges by automating the process and enhancing soft tissue visibility, leading to more reliable and efficient diagnoses.
Calcified Bone Detector Technology
How the Technology Works
A calcified bone detector uses a combination of artificial intelligence and advanced imaging techniques to identify and analyze calcified structures in medical scans. Deep learning models, especially convolutional neural networks (CNNs), process large volumes of imaging data. These models learn to distinguish between bone, soft tissue, and calcified regions with remarkable accuracy. Automated segmentation tools, powered by AI, further enhance the efficiency of the detection process. They reduce manual intervention and help radiologists focus on critical findings.
The table below highlights the technological advancements that drive these systems:
| Technology | Advancement | Impact |
|---|---|---|
| AI | Deep Learning (DL) | Enhances image analysis and diagnostic accuracy |
| Imaging Technologies | X-ray, DXA, CT, QCT, MRI | Improves diagnosis and management of osteoporosis |
| Automated Segmentation | AI-driven tools | Increases efficiency and reduces errors in diagnosis |
Detection Process Explained
The detection process begins when the calcified bone detector receives a medical image, such as an X-ray or CT scan. The software analyzes the image pixel by pixel, identifying patterns that indicate calcification. CNNs play a key role by providing high agreement levels and complete separation of categories, ensuring reliable results. The system then generates a report highlighting areas of concern for further review.
Clinical studies show that single-class models achieve a sensitivity of 0.98 and a precision of 0.91, while multi-class models reach a sensitivity of 0.88. These high scores demonstrate the reliability of the calcified bone detector in real-world settings.
Key Benefits of Calcified Bone Detector
Enhanced Soft Tissue Visibility
Calcified bone detector technology transforms the way radiologists view soft tissue structures. By digitally reducing the visual dominance of bones, this software allows for clearer observation of tissues that often remain hidden in traditional scans. Improved visibility supports the detection of subtle abnormalities, such as small tumors or lesions, that might otherwise go unnoticed.
The following table highlights how enhanced soft tissue visualization impacts the detection of underlying conditions:
| Evidence Description | Impact on Detection |
|---|---|
| Enhanced soft tissue visualization through decalcification and contrast agents like Lugol’s iodine | Improves visualization of soft tissue structures, aiding in the understanding of bone biology and pathology. |
| Decalcification reduces X-ray attenuation of bone | Allows for better contrast and detail in soft tissues, crucial for detecting underlying conditions. |
| Higher contrast-to-noise ratio (CNR) in soft tissues compared to bone | Facilitates detailed visualization of cellular structures, enhancing diagnostic capabilities. |
Radiologists can now identify and assess soft tissue changes with greater confidence. This improvement leads to more accurate diagnoses and better patient management.
Reduced Diagnostic Errors
Missed diagnoses often result from overlapping bone structures that obscure critical findings. Calcified bone detector software addresses this challenge by separating bone from soft tissue, which reduces the risk of oversight. Radiologists benefit from automated detection and clear visualization, which minimizes human error.
Tip: Consistent use of this technology helps radiologists catch subtle signs of disease earlier, reducing the likelihood of missed or incorrect diagnoses.
By providing a clearer view of the anatomy, the software supports more reliable interpretations. This accuracy is essential for early intervention and effective treatment planning.
Streamlined Workflow
Calcified bone detector systems not only improve image quality but also optimize the workflow for radiologists and imaging technicians. Automation reduces manual adjustments and repetitive tasks, allowing healthcare professionals to focus on clinical decision-making.
The table below outlines how this technology streamlines workflow:
| Feature | Benefit |
|---|---|
| Detection of CAC | Enhances diagnostic accuracy by identifying coronary artery calcification in non-contrast chest CT scans. |
| Integration into routine imaging | Maximizes findings from each scan, enabling early intervention and reducing unreported incidental findings. |
| Use of AI and machine learning | Ensures consistent imaging results, allowing radiologists to focus on actionable data without interference from normal anatomical structures. |
Radiology departments experience increased efficiency, faster turnaround times, and improved resource allocation. These advantages contribute to a smoother patient journey from imaging to diagnosis.
Improved Patient Outcomes
The ultimate goal of any medical imaging advancement is to improve patient outcomes. Calcified bone detector technology delivers on this promise by enabling more precise assessments and reducing unnecessary interventions. Clinical studies demonstrate significant benefits for patients, especially in the evaluation of coronary artery disease and other conditions involving calcified structures.
The following table summarizes clinical evidence supporting improved outcomes:
| Evidence Description | Result |
|---|---|
| Improved assessment of coronary artery disease (CAD) | 54% of patients reclassified to a lower disease category |
| Reduced overestimation of stenosis due to calcifications | Median degree of stenosis for calcified plaques: 29% vs. 42% |
| More accurate in-vitro quantification of stenoses | Significant changes in recommendations for over 50% of patients |
Patients receive more accurate diagnoses and tailored treatment plans. Early detection and proper classification of disease severity lead to better long-term health and reduced healthcare costs.
Using Bone Suppression Software: Step-by-Step
Installation and Setup
Installing bone suppression software begins with verifying system requirements. Technicians download the software package from the vendor’s secure portal. They follow on-screen prompts to complete the installation. Most vendors provide a guided setup wizard, which helps users configure initial settings. After installation, the system runs a diagnostic check to confirm compatibility with existing hardware. Support teams often offer remote assistance during this phase, ensuring a smooth start.
Tip: Always update the software to the latest version before integrating it with imaging systems. This step ensures access to the newest features and security patches.
Integration with Imaging Systems
Bone suppression software must work seamlessly with existing imaging platforms. Integration typically involves connecting the software to the hospital’s Picture Archiving and Communication System (PACS). Some systems, like OnGuard and SoftView, enhance cancer detection rates by improving tumor visibility. However, users may need to make manual adjustments for optimal performance. Real-time bone-suppressed images from 3D CT data remain unavailable in current solutions. Patient-specific weighting factors sometimes require manual tuning for best results.
| Integration Aspect | Compatibility Issue |
|---|---|
| Bone suppression algorithms improve tumor visibility in imaging systems. | Manual adjustments required for optimal performance. |
| Software like OnGuard and SoftView enhance cancer detection rates. | None of the systems provide real-time bone-suppressed images from 3D CT data. |
| RapidTrack software showed decreased tracking range error with BS images. | Manual adjustment of patient-specific weighting factors needed for optimization. |
Running Scans and Reviewing Results
Once integrated, radiologists select the bone suppression option before scanning. The software processes images automatically, generating both standard and bone-suppressed views. Radiologists review these images side by side, focusing on areas where bones might obscure soft tissue. The system highlights potential abnormalities, allowing for faster and more accurate diagnoses. Technicians can export results directly to the patient’s digital record, streamlining the workflow and supporting timely clinical decisions.
Common Challenges and Solutions
Managing False Positives and Negatives
Radiologists often encounter false positives and negatives when using calcified bone detector software. AI support can increase sensitivity in fracture detection, raising it from 0.67 to 0.80. However, the risk of false positives remains, especially in spinal fracture cases. Larger and more diverse training sets help improve accuracy. Many experts recommend using AI as a secondary tool for re-evaluating negative diagnoses. This approach reduces unnecessary follow-up procedures and enhances diagnostic confidence.
Tip: Regularly updating AI models with new clinical data can further minimize errors and improve reliability.
Training and Adoption
Successful adoption of bone suppression software depends on comprehensive training for radiologists and technologists. Skill variability among users can lead to inconsistent patient positioning and incorrect measurements. Maintenance lapses may cause calibration issues, affecting bone mineral density assessments. Structured education and ongoing learning opportunities address these gaps.
| Training Resource | Description |
|---|---|
| Integration of Artificial Intelligence in Radiology | Overview of AI integration in radiology practices. |
| Unlimited CE Credits | Access to unlimited continuing education credits for radiologists. |
| Radiology CE Credits | Specific continuing education credits for radiology professionals. |
| CE Webinars | Webinars focused on AI integration in radiology. |
| Webinar Replays | Access to recorded webinars for flexible learning. |
| Structured Education Credits | Credits for structured educational programs. |
| Exam Prep | Preparation resources for radiography and MRI exams. |
| Simplified Pathway Guides | Guides for certification pathways in radiology. |
Compatibility with Imaging Modalities
Bone suppression software enhances soft tissue visualization by suppressing structures like the rib cage in X-ray images. Its effectiveness varies across imaging modalities. The software performs well with X-rays but faces challenges in CT and MRI, where distinguishing between soft tissue and calcified structures proves more difficult. Consistent calibration and regular software updates help maintain compatibility and performance across different imaging systems.
Real-World Applications of Calcified Bone Detector
Clinical Success Stories
Hospitals and clinics have reported significant improvements in diagnostic accuracy after implementing calcified bone detector technology. Radiologists observed measurable gains in their ability to identify abnormalities. The following table presents data from five readers who used the technology in clinical settings:
| Radiologist | Accuracy Before | Accuracy After | AUC Before | AUC After | Misdiagnosis Ratio Before | Misdiagnosis Ratio After |
|---|---|---|---|---|---|---|
| Reader 1 | 89.7% | 92.3% | 0.927 | 0.937 | 11.5% | 7.6% |
| Reader 2 | 83.2% | 87.7% | 0.853 | 0.834 | 17.6% | 12.2% |
| Reader 3 | 79.4% | 92.3% | 0.825 | 0.878 | 21.4% | 7.6% |
| Reader 4 | 77.4% | 87.1% | 0.808 | 0.896 | 22.1% | 14.5% |
| Reader 5 | 63.2% | 83.2% | 0.694 | 0.846 | 35.9% | 16.0% |
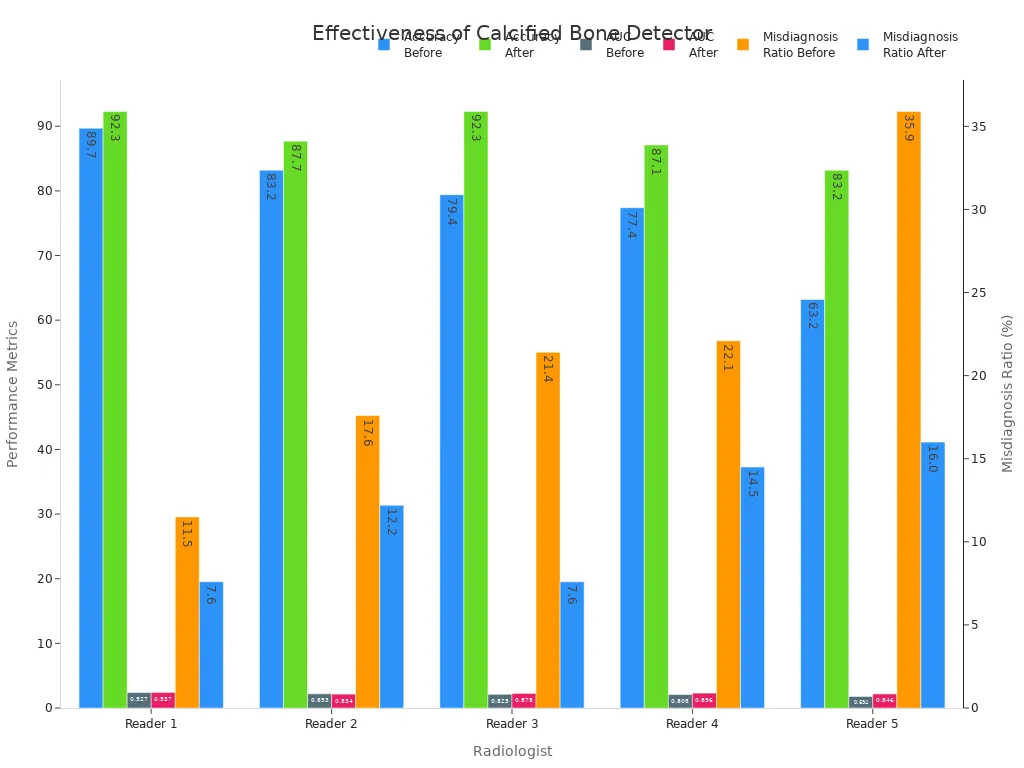
These results show that radiologists achieved higher accuracy and reduced misdiagnosis rates. Clinics reported faster turnaround times and fewer missed findings, which improved patient care.
Impact on Diagnostic Confidence
Calcified bone detector technology has increased diagnostic confidence among radiologists. Clinicians now report greater certainty when evaluating both positive and negative lung regions. The following table summarizes key findings from recent clinical practice:
| Evidence Type | Findings |
|---|---|
| Diagnostic Confidence | Increased mean confidence levels for both positive and negative lung regions with BSI |
| Variability | Reduced variability in confidence among readers |
| Reader Expertise | Improved diagnostic performance regardless of reader's expertise |
| Clinical Benefit | Particularly beneficial for less experienced clinicians and residents in emergency settings |
Radiologists with varying levels of experience benefit from more consistent results. Less experienced clinicians gain support in emergency situations, leading to better decision-making and improved patient outcomes.
Choosing the Right Calcified Bone Detector Software
Essential Features
Selecting the optimal calcified bone detector software requires careful evaluation of its core capabilities. Radiologists look for high sensitivity in detecting calcifications and robust segmentation tools. The software should offer seamless integration with existing imaging systems and support multiple modalities. User-friendly interfaces allow technicians to navigate workflows efficiently. Automated reporting and customizable alerts enhance clinical decision-making. Security features protect patient data and ensure compliance with healthcare regulations.
| Feature | Benefit |
|---|---|
| High Sensitivity | Detects subtle calcifications |
| Automated Segmentation | Reduces manual workload |
| Multi-Modality Support | Expands clinical utility |
| User-Friendly Design | Improves workflow efficiency |
| Data Security | Safeguards patient records |
Vendor Support and Updates
Reliable vendor support plays a crucial role in maintaining software performance. Vendors provide regular updates that address emerging clinical needs and security vulnerabilities. Dedicated technical support teams assist with troubleshooting and system optimization. Training resources help staff stay current with new features. Vendors who offer ongoing education and responsive service contribute to long-term success in clinical environments.
Tip: Choose vendors with a proven track record in healthcare technology and responsive customer service.
Cost and Value
Healthcare organizations assess both the upfront cost and the long-term value of calcified bone detector software. The incremental cost-effectiveness ratio (ICER) varies across machine learning models. Logistic Regression offers the most cost-effective solution, with a mean ICER of $278. Other models present higher ICERs, such as Random Forest at $412, RLS at $445, EN at $608, and SVM at $769. These procedural costs remain low compared to the significant improvement in quality-adjusted life years. The favorable cost-value relationship supports investment in advanced detection tools.
- Logistic Regression: ICER $278
- Random Forest: ICER $412
- RLS: ICER $445
- EN: ICER $608
- SVM: ICER $769
- Low procedural costs yield substantial gains in diagnostic outcomes
Calcified bone detector technology reduces missed diagnoses by accurately assessing bone strength and improving soft tissue visibility. Studies show strong agreement between imaging and mechanical tests, while bone suppression software increases diagnostic accuracy and sensitivity. Medical imaging departments benefit from adopting these advanced tools, paving the way for more reliable patient care.
| Evidence Description | Findings | Implications |
|---|---|---|
| Wald et al. study on distal tibia | Bone volume fraction and structural anisotropy indices predict mechanical competence with high accuracy | Supports the use of calcified bone detectors to avoid missed problems in imaging by accurately assessing bone strength |
| High-resolution micro-computed tomography | Good agreement between FE derived indices and mechanical test results | Validates the effectiveness of finite-element analysis in predicting structural integrity |
| Correlation with high-resolution CT imagery | Predicted mechanical indices from in vivo imaging correlate strongly with those from high-resolution CT | Reinforces the reliability of MRI and FE analysis in detecting issues in calcified tissues |
| Metric | Baseline Model | Bone-Suppressed Model | Statistical Significance |
|---|---|---|---|
| Matthews Correlation Coefficient (MCC) | Value A | Value B | p < 0.05 |
| Accuracy | Value C | Value D | p < 0.05 |
| Sensitivity | Value E | Value F | p < 0.05 |
| Specificity | Value G | Value H | p < 0.05 |
| Precision | Value I | Value J | p < 0.05 |
| F-measure | Value K | Value L | p < 0.05 |
FAQ
How does calcified bone detector software improve diagnostic accuracy?
The software highlights calcified regions and enhances soft tissue visibility. Radiologists can detect hidden abnormalities more easily, which leads to more accurate diagnoses.
Can hospitals integrate calcified bone detector software with existing imaging systems?
Hospitals can integrate most solutions with PACS and imaging platforms. Vendors often provide support and updates to ensure smooth compatibility and workflow.
Is calcified bone detector technology safe for patients?
- The technology uses existing scans.
- It does not require extra radiation or invasive procedures.
- Patients benefit from improved diagnosis without added risk.
See Also
Three Methods PHE Plates Enhance System Efficiency This Year
Key Capsule Checkweighers To Explore For Buyers This Year
The Importance Of Capsule Sorters In Eliminating Defects